Abstract
Background
In October 2020, we began the clinical trials of CD7 CAR-T treatment for CD7-positive hematological malignancies at our center. We found that the proliferation profile and evolution of CD7 CAR-T cells within 1-month following infusion into patients were quite different from those of CD19 CAR-T cells. From these data, we reasoned that the time to occurrence of CAR-T-cell-related side effects might also differ between the two cellular therapies. Here, we systematically compared the proliferation and CAR-T-cell-related side effects of CD7 CAR-T cells to these of CD19 CAR-T cells.
Patients and Methods
From October 2020 to June 2021, a total of 30 patients (24 male, 6 female) including 22 with T-cell acute lymphoblastic leukemia (T-ALL), 3 with T-cell lymphoblastic lymphoma (T-LBL), and 5 with mixed phenotype acute leukemia (MPAL) received autologous CD7 CAR-T cells manufactured by the SenlangBio company (https://clinicaltrials.gov NCT04572308, NCT04796441 and NCT04938115). The median follow-up time was 116 days (range: 15-221days). On Day 30, 25/30 patients (83.3%) achieved complete remission (CR)/CR with incomplete blood recovery (CRi). From December 2017 to June 2021, 45 B-ALL patients (19 male, 26 female) received CD19 CAR-T cells, also manufactured by SenlangBio (NCT04792593 and NCT04546893). The median follow-up time was 351 days (range: 15-1110days). On Day 30, 43/45 patients (95.6%) achieved CR/CRi.
The median infused CD7 CAR-T cell dose was 1×10 6/kg (range: 0.5-2×10 6/kg), and the median infused CD19 CAR-T cell dose was 3×10 5/kg (range: 0.2-10×10 5/kg). The CD7 or CD19 CAR-T cell ratio in peripheral blood lymphocytes (PBLC) and the CD7 or CD19 B-lymphocyte percentage in PBLC samples from patients were analyzed on days 0, 4, 7, 10, 14, 21, and 30 following CAR-T cell infusion using flow cytometry.
Results
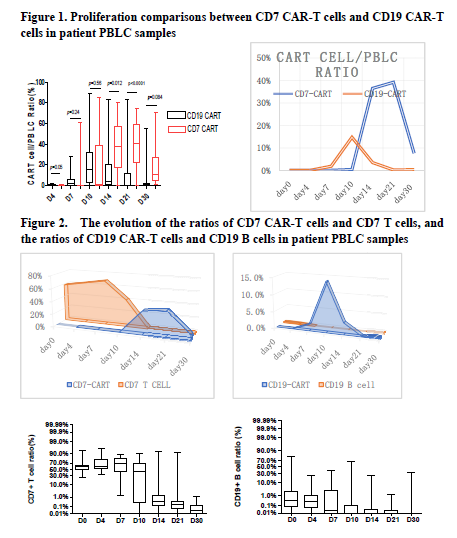
The presence of CD7 CAR-T cells in the PBLC samples were gradually detected following CD7 CAR-T cell infusion. The CD7 CAR-T cell ratio in PBLC increased significantly on Day 10. CD7 CAR-T cell peak appeared on Day 21 with a peak of 39.14% (range: 0.04%-74.58%), and was still detectable on Day 30 with a high CD7 CAR-T ratio of 7.5% (1.15%-70.41%). The ratio of CD19 CAR-T cells in patient PBLC samples showed a significant increase on Day 7 following infusion, and the CAR-T cell peak appeared on Day 10 with a peak of 14.71% (range: 0.11%-89.33%), and then quickly decreased to 0.23% (range: 0%-82.88%) on Day 21 (Figure 1). As the CAR-T cells increased, the proportion of target cells decreases significantly (Figure 2). However, the rate of decrease of CD19 cells differed from that of CD7 cells.
CAR-T cell proliferation is also associated with CAR-T-cell-related adverse effects including cytokine release syndrome (CRS) and immune effector cell-associated neurotoxicity syndrome (ICANS). Observing the adverse effects after CD7 CAR-T infusion, we found that fever (incidence rate of 83.8%) occurred on the first 1-3 days following infusion, with a body temperature among patients of about 38°C. After patients' body temperature dropped to approximately normal levels, fever occurred again on Day 10-21 (incidence rate of 77.4%), and a higher temperature of 38-40°C was observed. The adverse event profile coincided with the proliferation of CD7 CAR-T cells we observed. Among the 30 cases, 5 had Grade 2 CRS, 2 had CRS of Grade ≥3, and 1 patient had Grade 3 ICANS. Fever following CD19 CAR-T infusion consisted mainly on Day 7-14 after the infusion (incidence rate of 86.6%), followed by a gradual drop of body temperature to normal after Day 14. Among the 45 patients, 5 had Grade 2 CRS, 5 had CRS of Grade ≥3 and 7 had Grade ≥3 ICANS.
Conclusions
In this clinical study, we found that the proliferation and evolution of CD7 CAR-T cells are distinct from that of C19 CAR-T cells. CD7 CAR-T cells began to proliferate significantly later following patient infusion and persisted longer compared to CD19 CAR-T cells. We found that patients experienced two rounds of fever, appearing on Day 1-3 and Day 10-21 following CD7 CAR-T infusion, which required more attention and prevention compared to the fever experienced by patients infused with CD19 CAR-T cells. However, the incidence of CRS and ICANS did not increase following CD7 CAR-T infusion. More patients and long-term observation are needed to confirm these results and to improve clinical management of patients treated with CAR-T cellular therapies.
No relevant conflicts of interest to declare.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal